
Obsessive-Compulsive Disorder (OCD)
Specialised assessment and treatment of Obsessive-Compulsive Disorder in Lisbon
WHAT IS OCD?

An exhaustive cycle of thought and action
OCD (Obsessive-Compulsive Disorder) is a serious and, unfortunately, common psychiatric condition. It is not a simple "craze" for organisation or cleanliness, but a neurobiological dysfunction in which the brain becomes trapped in a continuous cycle of intrusive thoughts that cause enormous suffering, leading the person to perform repetitive behaviours to relieve that same anguish.
Most common manifestations
- ObsessionsIntrusive and unwanted ideas, images or impulses (e.g. irrational fear of contamination, constant doubts or catastrophic fears).
- Compulsions (Rituals)Physical behaviours or repetitive mental acts performed to neutralise the anxiety caused by obsessions.
- The Relief TrapThe compulsion brings temporary relief, but in the long term it reinforces the obsession, perpetuating the vicious cycle of OCD.
- Functional ImpactRituals take up a lot of time (often hours a day), jeopardising work, studies, relationships and all spheres of life.
MAIN MANIFESTATIONS OF TOC
Contamination and washing
Irrational fear of germs, disease or dirt, resulting in compulsions to wash hands, body or house excessively.
CleaningDoubt and Verification
Constant worry that something bad will happen (e.g. leaving the cooker on, the door open), leading to repeated checks.
VerificationSymmetry, Order and Counting
Extreme need for objects to be perfectly aligned, symmetrical, or grouped in the "right" number.
OrganisationIntrusive Thoughts
Disturbing images or thoughts, sometimes of an aggressive, religious or sexual nature, resolved through mental acts ("pure OCD").
Purely Obsessive OCD
OCD can take many forms and symptoms can vary over time if not treated properly.
EFFECTIVENESS IN TREATMENT
OCD
Clinical results consistent with the most advanced methodologies in psychiatry and neuromodulation
* Therapeutic success varies according to severity, comorbidities and adherence to treatment. OCD is a chronic condition that benefits from ongoing monitoring.
Sources: clinical data, Öst et al. (2016) - Meta-analysis of CBT for OCD; Carmi et al. (2019) - Real-world efficacy of dTMS for OCD (22 clinical centres); FDA (2018) - Approval of dTMS for OCD; Eisen et al. (2013) - Meta-analysis of longitudinal studies, remission and recurrence; APA Guidelines for OCD.
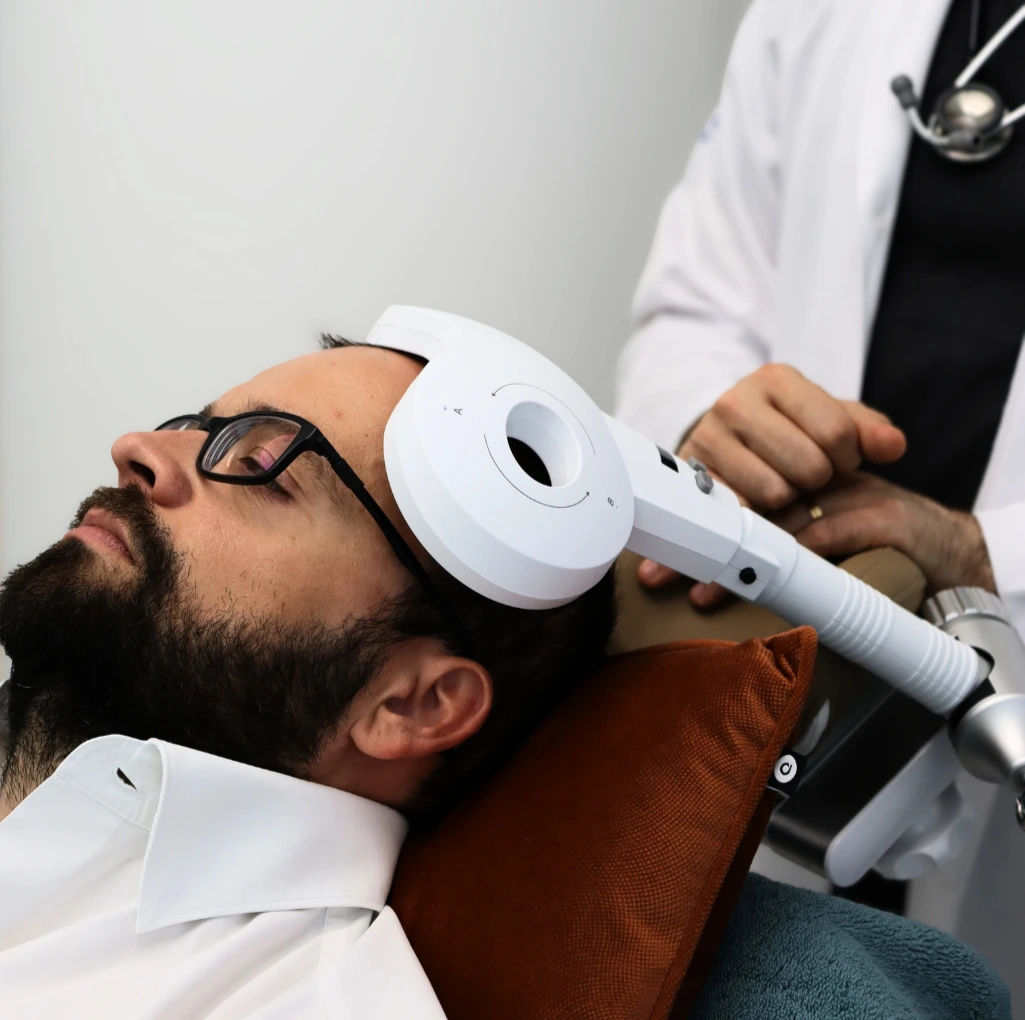
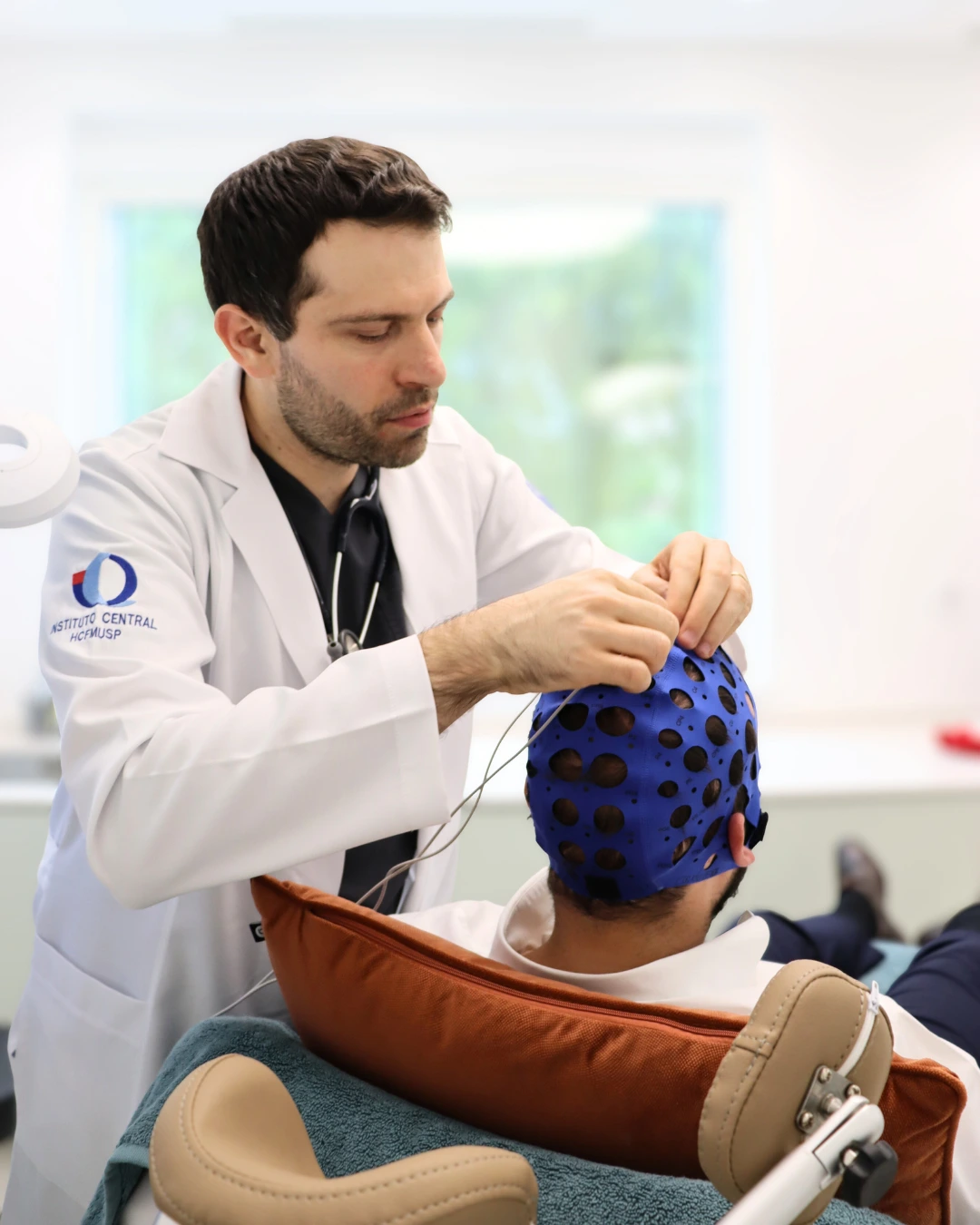
TECHNOLOGY AND THE THERAPEUTIC ENVIRONMENT



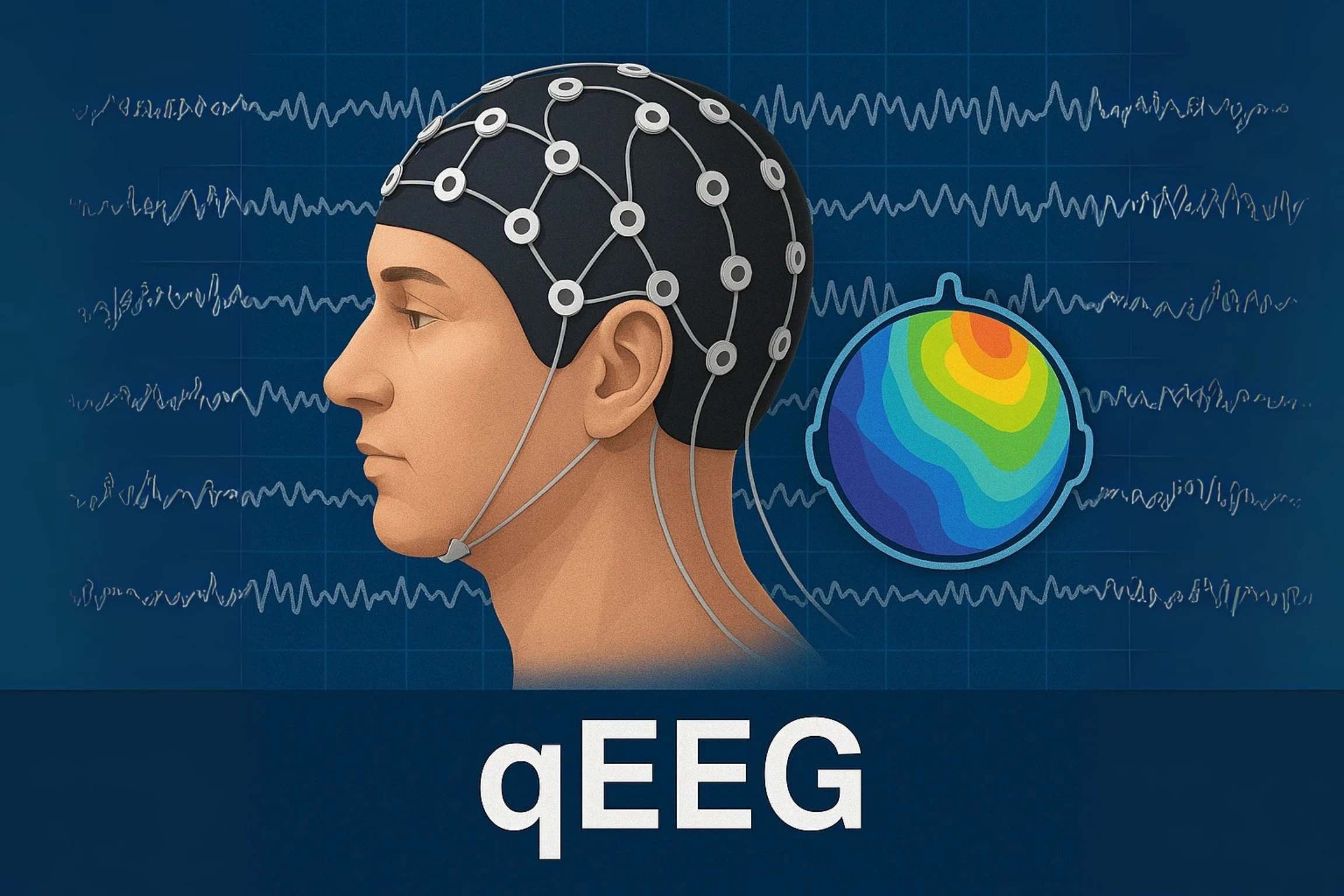


THE IMPORTANCE OF DIAGNOSIS AND TREATMENT
OCD is often concealed by sufferers due to shame or fear of misunderstanding, often delaying diagnosis for several years. It is essential to realise that this is not a personality problem or character flaw, but a neuropsychiatric dysfunction that needs and receives appropriate medical treatment.
At NeuroPsyque, we apply protocols based on the most robust clinical evidence. We combine pharmacological support with Cognitive Behavioural Therapy with Exposure and Response Prevention (ERP). For the most severe cases that are resistant to conventional drugs, we use Transcranial Magnetic Stimulation (TMS), which has been widely proven to be effective in the brain circuits affected by OCD.
FAQ's about OCD
What's the difference between "having manias" and having OCD?
What causes OCD?
Is there a definitive cure for OCD?
How does EPR Cognitive Behavioural Therapy work?
Is neuromodulation (EMT) indicated in OCD?
Can OCD manifest itself only with thoughts, without physical actions?
Do I need a medical referral to book an appointment at NeuroPsyque?
Free yourself from the cycle of obsessions
Book your specialised appointment today and take back control of your life.
To provide the best experience, we use technologies such as cookies to store and/or access device information. Consenting to these technologies will allow us to process data such as browsing behaviour or unique IDs on this website. Not consenting or withdrawing consent may negatively affect certain features and functions.
