The Complete Guide to Understanding, Diagnosing and Treating
It is estimated that neuropathic pain affects 7-10% of the European population, but in Portugal many cases remain underdiagnosed. Is it just "a stronger pain"?
 Imagine waking up every morning with the feeling that thousands of needles run through your legsor that a hot iron is constantly pressed against your skin. It's not a pain that comes and goes - it's a constant presence, a burning that won't stop even when there is no visible wound.
Imagine waking up every morning with the feeling that thousands of needles run through your legsor that a hot iron is constantly pressed against your skin. It's not a pain that comes and goes - it's a constant presence, a burning that won't stop even when there is no visible wound.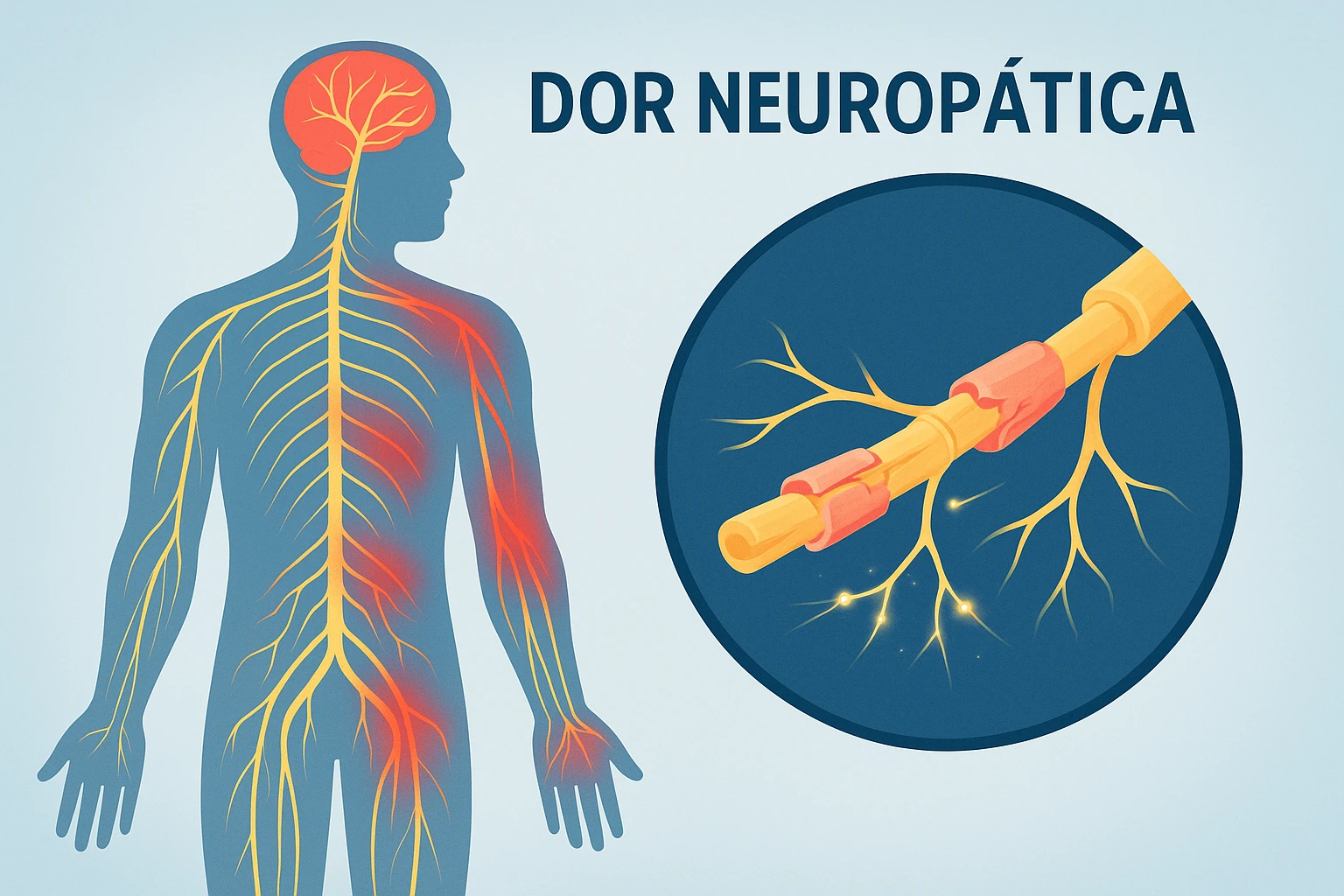
🕒 Table of Contents
- 1. 🧠 What is Neuropathic Pain?
- 2. 📊 Difference between Neuropathic Pain and Other Pains
- 3. 🤕 Most common symptoms of neuropathic pain
- 4. Types of Neuropathic Pain
- 5. ⚠️ Causes and risk factors
- 6. The Diagnosis of Neuropathic Pain?
- 7. 📉 Impact of neuropathic pain on daily life
- 8. 💊 How is neuropathic pain treated?
- 9. When to seek professional help
- 10. 🧘♀️ How to deal with Neuropathic Pain in everyday life?
- 11. 🔬🚀 Advances in scientific research
- 12. 🤔 Myths and Truths about Neuropathic Pain
- 13. 🇵🇹🤝 Resources and support available in Portugal
- 14. Conclusion
- 15. ❓ FAQ's on Neuropathic Pain
What is Neuropathic Pain?
Neuropathic pain is pain that results from a lesion or problem in the nervous system. It's very different from the common pain we all know.
When you cut your finger or hit your knee, you feel pain. This is because the pain receptorsPain in the finger or knee sends alarm signals to the brain. We call this normal pain nociceptive - is a response that protects us, alerting us to danger.
In neuropathic painThe nervous system itself is damaged. It's as if the body's "alarm system" has short-circuited. It sends out pain signals even when there is no real danger. The result is painful sensations that usually don't go away. They are often described as burning, electric shocks or intense tingling.
Medical definition
According to IASP (International Association for the Study of Pain), is pain caused by injury or disease of the nerves responsible for sensation. It is also classified as such by WHOin the reference guide ICD-11. In short, the cause of the pain is internal to the nervous system, not external, such as a cut or a blow.
A burning pain, for example, happens when the pain nerves become active for no reason. The feeling of shock comes from abnormal electrical signals in damaged nerves.
This condition can affect any part of the body, manifesting itself in a wide variety of ways. For this reason, diagnosis is a challenge even for specialised professionals.
Difference Between Neuropathic Pain and Other Pains
To truly understand neuropathic painIt is essential to realise exactly how it differs from other types of pain, which can mean other problems:
| Character. | Nociceptive pain | Neuropathic Pain |
| Cause | Identifiable tissue damage | Nervous system dysfunction |
| Type | Stinging, aching | Burning, shocks, tingling |
| Localisation | Well located | Localised or diffuse |
| Response to drugs | Variable (good) | Limited response |
| Duration | Temporary | Undefined |
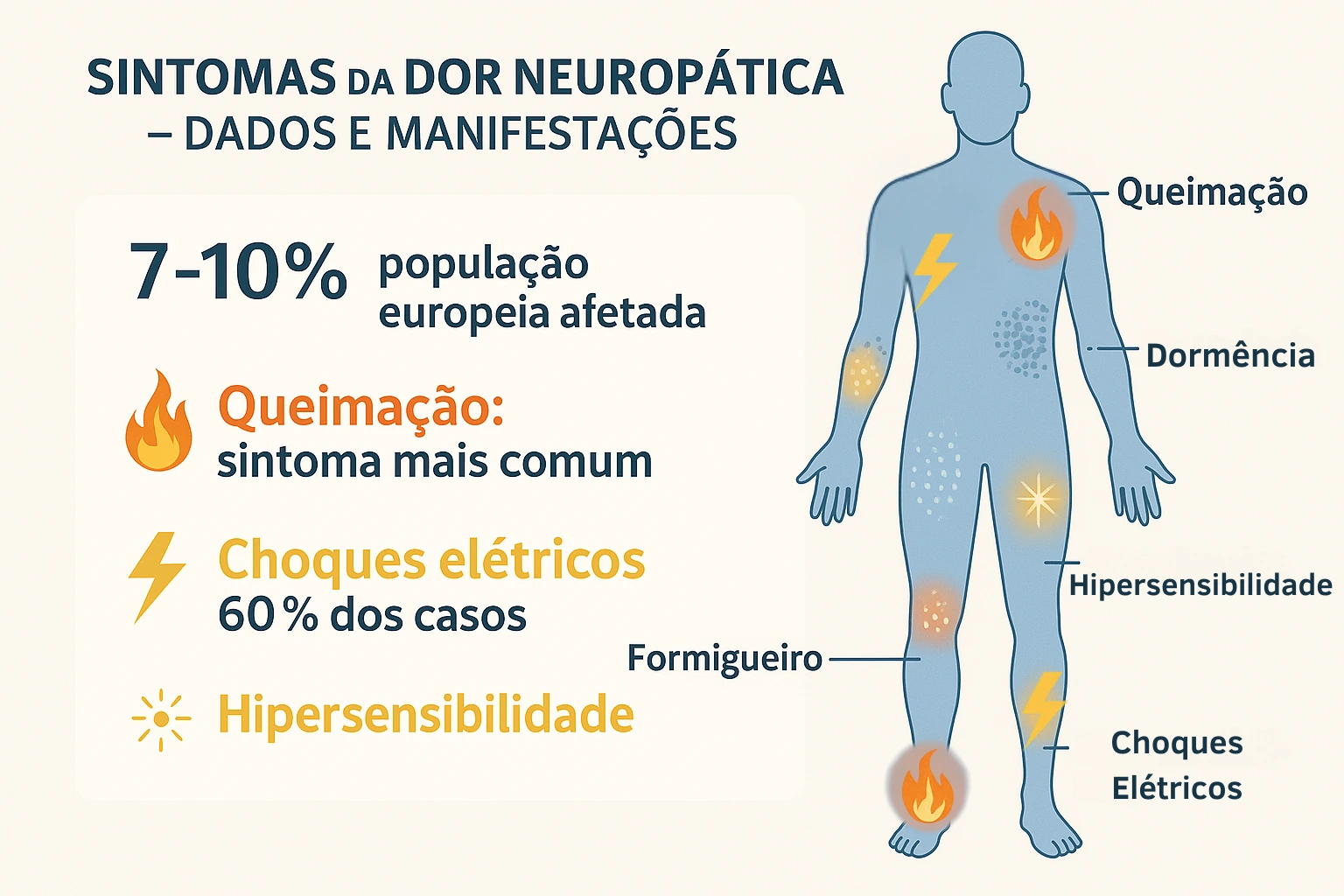
Most common symptoms of neuropathic pain
Neuropathic pain manifests itself through various symptoms.
Patients often describe their experiences in very specific ways:
Burning sensations
"As if I had acid on my skin"
"A constantly leaning hot iron"
"Skin burning from the inside"
Electric shocks
"Discharges that go through the body"
"Constant shocks"
"Sudden and intense needles"
Tingling or Numbness (Paresthesia)
"Persistent tingling or numbness"
"Thousands of needles pricking"
"Numbness with burning" (dysaesthesia)
Hypersensitivity to touch (Mechanical Allodynia)
- Pain caused by normally non-painful stimuli
- A gentle touch or rubbing of clothing can cause intense pain
Reduced sensitivity (Hypoaesthesia)
"My skin feels like it's covered in a film"
"I don't perceive heat or cold as I used to"
"The area seems disconnected from the body"
Increased pain (Hyperalgesia)
- Exaggerated response to painful stimuli
- A little pinch can feel like a cut
Other common symptoms:
Pain that gets worse at night
Feeling of "dead" or strange skin
Difficulty distinguishing temperatures
Pain that spreads to areas not initially affected
Neuropathic pain can cause extra sensations (hyperaesthesia), but also fewer sensations (hypoaesthesia). Both phenomena indicate that there are changes in the functioning of the nerves.
Important Note:The presence of these symptoms does not automatically confirm neuropathic pain. The diagnosis should always be made by a specialised professional who can assess the whole picture.
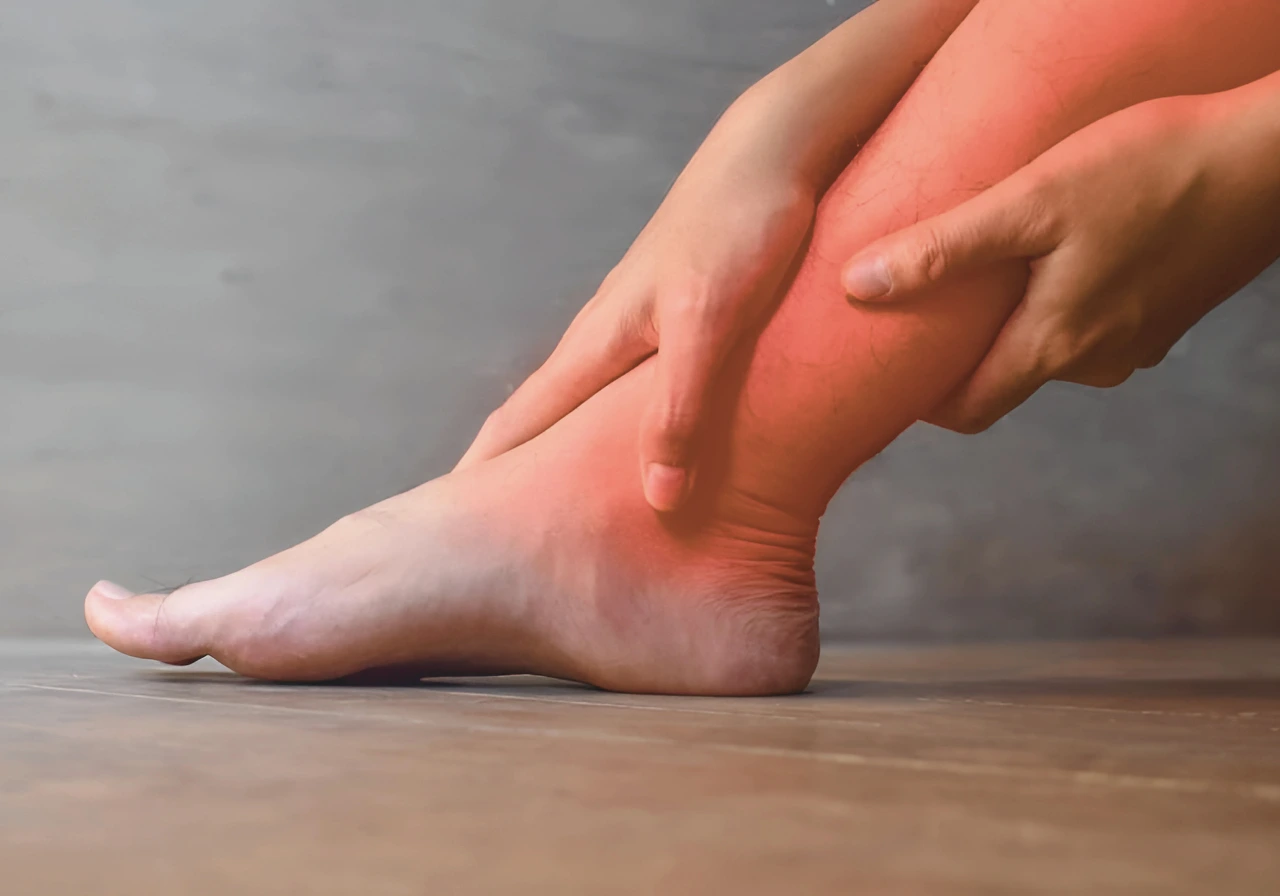
Types of Neuropathic Pain
Neuropathic pain can be categorised in various ways, helping to guide treatment:
Peripheral or Central
The nervous system is divided into the central nervous system and the peripheral nervous system.
- Peripheral Neuropathic Pain
- It develops after an injury or illness that affects only the peripheral somatosensory nervous system - responsible for receiving and processing sensory information from the body, such as touch, temperature, pain and proprioception (spatial awareness of the body's position). Examples include diabetic neuropathy, post-herpetic neuralgia, or the severing of a nerve.
- Central Neuropathic Pain
- It results from an injury or disease of the central nervous system (CNS), and often occurs after a stroke, spinal cord injury or demyelinating plaque from multiple sclerosis.
Localisation of the lesion
- Mononeuropathy
- Only one nerve pathway is compromised. The pain is well localised.
- Polyneuropathy
- When several nerves are altered, the pain is generalised and can appear in the trunk, arms and legs simultaneously.
Time pattern
- Spontaneous pain
- Continuous (persistent burning)
- Paroxysmal (sudden electric shocks)
- Evoked pain
- Pain caused by normally non-painful stimuli (allodynia)
- Exaggerated pain to painful stimuli (hyperalgesia)
Causes and risk factors
Neuropathic pain can result from various conditions that affect the nervous system:
Diabetes
The most common type of peripheral neuropathic pain is painful diabetic peripheral neuropathywhich affects 60-70% of people with diabetes. High blood sugar progressively damages the peripheral nerves.
Viral infections
- Viruses like Herpes zoster (zone) can cause post-herpetic neuralgia
- 33% of patients with HIV/AIDS infection develop neuropathic pain
Trauma and surgery
Accidents, fractures or surgery can cause nerve damage that leads to acute, high intensity pain. The pain can persist long after the tissues have healed.
Chemotherapy
30-40% of cancer patients undergoing chemotherapy develop neuropathic pain due to the toxic effects of drugs on the nerves.
Autoimmune diseases
- Multiple sclerosis
- Rheumatoid arthritis
- Sjögren's syndrome
Other factors:
- Alcoholism and nutritional deficiencies
- Nerve compression (herniated discs...)
- Degenerative neurological diseases
- Certain medicines
Risk factors
Some factors increase the probability of developing neuropathic pain:
- Older age
- Poorly controlled diabetes
- Family history of neuropathies
- Excessive alcohol consumption
- Vitamin deficiencies (especially B12)
- Exposure to toxins

The Diagnosis of Neuropathic Pain
The clinical examination is very important for correctly diagnosing the type of pain. It includes talking to the patient and carrying out physical examinations of the nerves.
The diagnosis of neuropathic pain is mainly made through analysing symptoms e neurological physical examinationsfeedback analysis. There is no single test to confirm the condition.
The diagnostic process includes:
Detailed medical history
- Analysing the clinical history
- Precise description of pain and symptoms
- Onset and evolution of symptoms
Neurological physical examination
- Sensitivity assessment
- Reflex tests
- Muscle strength assessment
- Specific tests for allodynia and hyperalgesia
There are also tools such as standardised questionnaires, like the questionnaire DN4 or the LANSS scale, which help to identify neuropathic pain characteristics.
DN4 Questionnaire
DN4 evaluates 10 signs and symptomsdivided into two parts:
1. Symptoms reported by the patient (7 items)
(Answers: Yes/No)
Feeling of burning
Feeling of electric shocks
Feeling of anthill
Feeling of pinpricks
Numbness
Itching/pruritus
The pain is caused by a light touch (allodynia)
2. Clinical signs assessed during the physical examination (3 items)
(Answers: Yes/No)
Hypoaesthesia to touch (sensation reduced to the touch with cotton)
Hypoaesthesia to the bite (sensation reduced when pricking with a needle)
The pain is caused by rub of a light object (e.g. cotton) - tactile allodynia
Interpretation of results
Every "Yes" answer is worth 1 point
A score ≥ 4 (equal to or greater than 4) indicates high probability of neuropathic pain
Additional diagnostic criteria
To be considered neuropathic pain, must be present:
- Plausible neuroanatomical distribution:
pain must follow the distribution pattern of specific nerves - History suggestive of nerve damage:
there must be evidence of disease or injury affecting the nervous system - Confirmation tests:
tests such as electroneuromyography can confirm nerve dysfunction
Complementary examinations when necessary:
- Electroneuromyography
- Magnetic resonance imaging
- Skin biopsy (specific cases)
- Nerve function tests
Important Note:A neuropathic pain is difficult to recognise and is therefore a health condition that is considered underdiagnosed. It is essential to seek out professionals with experience in this area.
Impact of Neuropathic Pain on Daily Life
Neuropathic pain is a reason for suffering e disability for many patients, constituting a public health problem.
The impact goes far beyond physical pain, affecting multiple dimensions of life:
Physical impact
Reluctance to move the painful part of the body, resulting in muscle atrophy, joint ankylosis (stiffness) and limited movement
Sleep disorders due to nocturnal pain
Chronic fatigue
Reduced general functional capacity
Psychological impact
Pain, and especially chronic pain, is often accompanied by symptoms of depression and anxiety. Nature "invisible" neuropathic pain can aggravate psychological suffering.
- Constant anxiety
- Reactive depression
- Frustration and irritability
- Loss of self-esteem
- Feeling misunderstood
Social and family impact
- Significant consequences for families and the social environment
- Social isolation
- Difficulties in the marital relationship
- Overburdened carers
- Misunderstanding by others
Professional impact
- Time off work
- Reduced productivity
- Frequent absences
- Early retirement due to disability
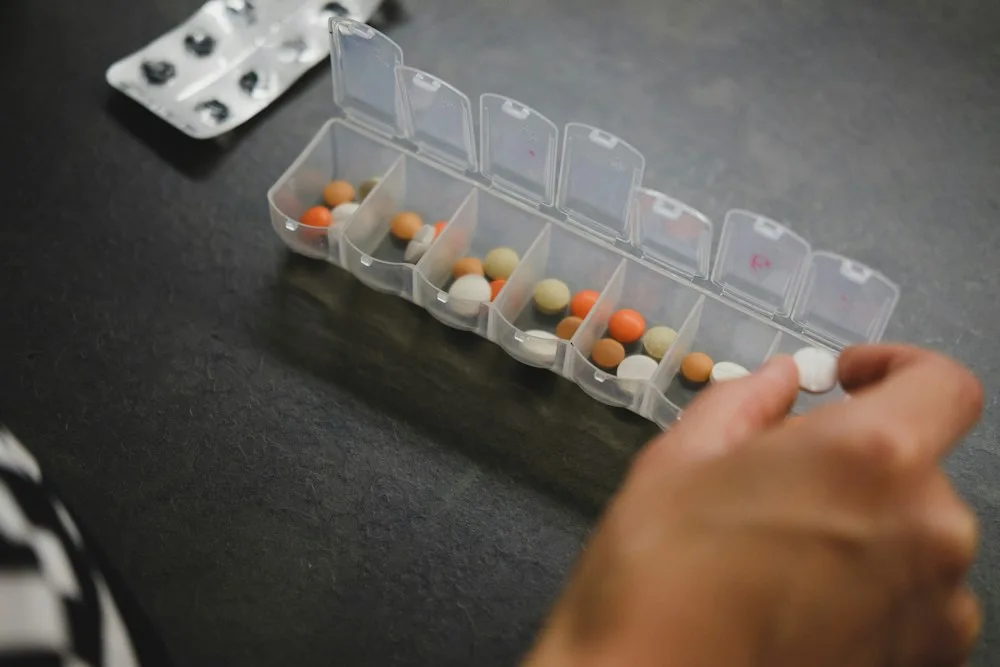
How is Neuropathic Pain treated?
Various classes of drugs have some efficacy, but complete relief is unlikelyIt is important to set realistic expectations regarding medication. The aim of pharmacological treatment is to reduce neuropathic pain, so that it can be reduced. less debilitating and therefore, hardly helps to treat the "root" causing the pain.
Treatment of neuropathic painfor the best possible expectation of improvement, requires an approach integrated multidisciplinary approach, combining different therapeutic strategies:
Medicines used for treatment
Gabapentinoids (first line)
- Pregabalin
- Gabapentin
Antidepressants
- Tricyclicsamitriptyline, nortriptyline
- Dualsduloxetine, venlafaxine
Topical medicines (ointments, gels)
- Lidocaine
- Capsaicin in high concentration
Important Note:
Opioid analgesics can provide some relief, but are generally less effective than for acute nociceptive pain and are associated with the risk of addiction.
Neurotherapy's role in treatment
A Neurotherapy represents an effective approach to treating neuropathic pain:
- Transcranial Magnetic Stimulation (EMT)
EMT modulates the prefrontal cortex, which stimulates other regions of the brain, helping to restore the pain-free condition.- No significant side effects
- Acts to modulate pain perception
- Studies show changes in neuronal activity in regions involved in pain regulation
- Neurofeedback (NF/qEEG)
- Trains the brain to better process pain signals
- Improves neuronal self-regulation
- Effectively complements other treatments
- Transcranial Direct Current Stimulation (tDCS)
- Shows promising results in modulating pain and mood
- Safe and well-tolerated technique
In NeuroPsyqueWe use an integrated approach that combines advanced neurotherapy with specialised neurological careOur services are tailored to the specific needs of each patient. Our focus is to offer the best possible expectation of improvementusing state-of-the-art technologies with a safety profile superior to conventional pharmacological treatments.
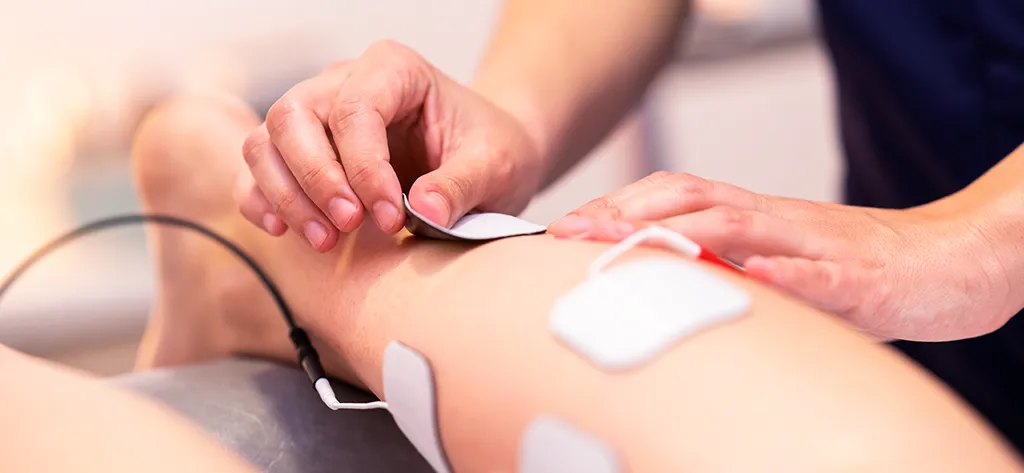
When to seek professional help
It is essential to seek specialised assessment when:
- Identify various symptoms listed in the test DN4explained above
- Pain doesn't improve with conventional painkillers
- The pain gets progressively worse/worse
- Symptoms persist for more than 3 months
Early diagnosis and appropriate treatment can prevent the condition from worsening and significantly improve quality of life.
How to deal with Neuropathic Pain in everyday life?
In addition to specialised medical care, there are strategies that can improve quality of life:
Pain management
- Relaxation and deep breathing techniques
- Application of heat or cold (according to tolerance)
- Gentle massage on non-hypersensitive areas
- Meditation and mindfulness
Sleep care
- Keeping regular hours
- Create a comfortable environment
- Avoid caffeine and screens before going to bed
- Consider positions that reduce pressure on painful areas
Adapted physical activity
- Low-impact physical exercise, prescribed by the Physiotherapist
- Hydrotherapy
- Gentle stretches
Stress management
- Maintaining hobbies and pleasurable activities
- Participation in support groups
- Talking about the condition with family and close friends
General care
- Protection of hypersensitive areas
- Wear soft, non-tight clothing
- Special care with temperature
- Proper nutrition - B vitamins are important

Advances in scientific research
Research into neuropathic pain is constantly evolving, bringing new hopes for patients. Here are some of the most promising advances:
Medical cannabis in treatment
A cannabis represents a promising therapeutic approach for the treatment of neuropathic pain, a condition often resistant to conventional treatments.
Neuromodulation and new treatments
- Advanced stimulation techniques
- Stimulation of peripheral nerves can interrupt pain signals travelling through the nerves, providing relief to patients with localised neuropathic pain (study)
Biomarkers and personalised medicine (study)
- Identification of genetic profiles
- Biomarkers of response to treatment
- Targeted therapies based on pain phenotype (type)
Regenerative therapies (study)
- Neural growth factors
- Stem cell therapy
- Regenerative medicine for peripheral nerves
Myths and Truths about Neuropathic Pain
It is essential to clear up misconceptions about this condition:
| Myth | Truth |
| "The pain is only in the head" | Neuropathic pain has a real neurobiological basis and can be measured through specific tests. |
| "Pain medication solves the problem" | Conventional analgesics and anti-inflammatories have limited efficacy in neuropathic pain, and specific treatments are needed. |
| "It's a rare condition" | It affects 7-10% of the European population and is more common than you might think. |
Resources and support available in Portugal
Portugal has several organisations and resources to support people with neuropathic pain:
| Resource | Description |
| APED - Portuguese Association for the Study of Pain | Leading organisation in promoting knowledge about pain in Portugal |
| SIP Portugal | Platform that brings together health professionals and patient organisations |
| SNS 24 line | 24-hour telephone support: 808 24 24 24 |
| Hospital Pain Units | 22 specialised units throughout the country |
| DOR.com | Site dedicated to Pain |
In NeuroPsyqueWe are part of a network of specialised care, offering a response that combines Neurology, Neurotherapy e Physiotherapy. Our commitment is, as always, to provide you with the greatest possible expectation of improvement.
We have Transcranial Magnetic Stimulation, Neurofeedback e Transcranial Direct Current Stimulationwhich have proved important in the treatment of neuropathic pain. Book your appointment with us!
Conclusion
A neuropathic pain is a complex condition that affects millions of people worldwide, including hundreds of thousands in Portugal. Although it represents a significant challenge, it is important to emphasise that it's not a sentence of permanent suffering.
Scientific advances in recent years have brought new treatment prospects - from more effective drugs to neuromodulation, the therapeutic options continue to expand. The expansion of knowledge about genetics brings promising possibilities, and the Transcranial Magnetic Stimulation shows efficacy in modulating pain perception.
The key to success lies in early diagnosis and specialised treatment. Each person is unique, and finding the ideal therapeutic combination may take time and adjustments, but it's worth persevering.
If you live with symptoms that might suggest neuropathic paindon't hesitate to seek specialised help. Silent suffering has no place. Book your appointment with us!
FAQ's on Neuropathic Pain
1. Can neuropathic pain be cured?
Although there is no definitive "cure" for all forms of neuropathic painThe symptoms can be very well controlled with appropriate treatment. The aim is to reduce the pain so that it is less debilitating, allowing for a normal and productive life.
2. What are the most characteristic symptoms?
The most common are continuous burning pain, shock sensations and mechanical allodynia. Patients often describe sensations of a "hot iron", "electric shocks" or "thousands of needles".
3. How is the diagnosis made?
Diagnosis is based mainly on anamnesis and neurological physical examination. There is no specific test, but questionnaires such as the DN4 and complementary tests (electroneuromyographymagnetic resonance imaging) can support the diagnosis.
4. Is neurotherapy effective for neuropathic pain?
Yes, techniques such as Transcranial Magnetic Stimulation have shown promising results in modulating pain perception. Neurotherapy represents a lower risk alternative to pharmacological treatments, acting on the neuroplasticity.
5. How long does the treatment take?
The time varies according to the individual case. Medications can take 6-12 weeks to show full effect. Neurotherapy can show benefits more quickly, but requires regular sessions for lasting results.
6. Can I work with neuropathic pain?
With appropriate treatment and possible adaptations in the workplace, many people are able to maintain their professional activity. The important thing is to seek specialised support to optimise symptom control.
7. Can neuropathic pain get worse over time?
Without proper treatment, symptoms can intensify. However, with specialised monitoring and appropriate treatment, it is possible to stabilise or even improve the condition.
8. Are there support groups in Portugal?
Yes, there are various associations and support groups for sharing experiences about chronic pain. Some resources are listed above!
9. How do I explain the condition to my family?
Show them this article! It's important to educate family members about the reality of neuropathic pain, emphasising that pain is real even without visible external signs. Educational materials and participation in consultations can help with understanding.
10. Does physical exercise help or harm?
Adapted and gradual exercise can be beneficial, but it should be guided or prescribed by a specialised physiotherapist. Physical activity helps to prevent muscle atrophy and maintain range of movement, but must respect individual limits.
11. What are the side effects of the medicines?
Gabapentinoids (pregabalin, gabapentin) can cause drowsiness, dizziness, weight gain and oedema. Antidepressants can affect sleep and appetite.