The Complete Guide to Understanding, Diagnosing and Treating

In Portugal, 28.1% of the population over 18 suffer from insomnia symptoms at least three nights a week. In the over-65s, this figure rises to an alarming 50%. But is insomnia just a question of "not being able to sleep"?
It's 2.30 in the morning and you're lying there, eyes open, mind spinning in endless circles of worries. Your body is tired, but your head seems to have a life of its own - an internal conversation that you can't stop. He looks at the alarm clock: it's four and a half hours away. She closes her eyes tightly, tries to take a deep breath, counts sheep. Nothing. Frustration grows: "Why can't I just go to sleep?"
For millions of Portuguese, this is not an occasional experience - it's a never-ending cycle. Insomnia is not laziness, lack of discipline or "thinking too much". It's a real medical condition that fundamentally alters the way the brain manages sleep and wakefulness.

🕒 Table of Contents
- 🧠1. What is Insomnia?
- ↔️2. Difference between Insomnia and "Bad Night's Sleep"
- 🤕3. The most common symptoms of insomnia
- 📍4. Types of Insomnia
- 🧬5. Causes and risk factors
- 🩺6. Diagnosing Insomnia
- 📉7. The impact of insomnia on daily life
- ⚠️8. The Real Impact of Sleep Deprivation - examples
- 💊9. How is Insomnia treated?
- 🧘10. The Science of Healthy Sleep - A Practical Guide
- 🆘11. When to seek professional help
- 🔬🚀12. Advances in scientific research
- 🤔13. Myths and Truths about Insomnia
- 🤝14. Resources and support available in Portugal
- ✨15. Conclusion
- ❓16. Questions and answers about Insomnia
What is Insomnia?
Insomnia is the persistent difficulty in initiating and maintaining restful sleep. It's a sleep disorder more frequent in adults, and greatly affects quality of life and daily functioning.
Contrary to popular belief, insomnia is not just "having trouble falling asleep". People with insomnia often report even when they can sleep, they wake up tired.
Medical Definition
According to International Classification of Sleep Disorders (ICSD-3)Insomnia is characterised by:
- Difficulty initiating sleep, maintaining it, or both
- Non-restorative sleep, despite adequate opportunity to sleep
- Impairment of daily, functional well-being
If at least 3 times a weekfor a minimum of 3 monthsa diagnosis of chronic insomnia.

Recognition in Portugal
In Portugal, insomnia is officially recognised as a public health problem. In a general practitioner's consultation, around 69% of patients, more than 2 in 3, have symptoms of insomnia. Many Portuguese suffer in silence or out of habit, without seeking specialised help.
Portugal is alarmingly OECD country with the highest consumption of sleeping pills. This is a worrying indicator. Even if the cases come to the doctor's office, treatments are not conclusive. Medicines often do not solve the problem permanently, but almost always create another one - dependence.
Important Note:Insomnia it's never normalregardless of age. Variations in sleep are normal throughout life. But constant difficulty sleeping is always a problemYou need a specialised assessment, no matter how old you are.
The difference between insomnia and a "bad night's sleep"
We've all had the occasional night when we sleep badly. This is normal, and usually the result of one-off situations such as the physical and/or mental stress. Insomnia is different.
| Features | Bad Night's Sleep | Insomnia |
| Frequency | Occasional | At least 3 nights/week |
| Duration | A few days | Minimum 3 months (chronic) |
| Daily impact | Minimal, temporary | Significant, persistent |
| Control | Resolves spontaneously | Requires specialised intervention |

Most common symptoms of insomnia
Nocturnal symptoms:
- Taking more than 30 minutes to fall asleep every day
- Waking up many times during the night
- Waking up too early and not being able to get back to sleep
- Feeling of superficial, non-restorative sleep
Daytime symptoms:
- Persistent fatigue even after enough hours in bed
- Concentration and memory difficulties
- Irritability and mood swings
- Drowsiness during daily activities
- Reduced professional income
Types of Insomnia
Acute vs chronic insomnia
Acute Insomnia (Transient):
- Duration of less than 3 months
- Usually related to situational stress
- Causes: exams, family problems, debts, job changes, bereavement
- Often solved by eliminating the problem that caused it
- It affects almost everyone at some point in their lives
Chronic Insomnia:
- Duration of more than 3 months
- Occurs at least 3 nights a week
- More complex, diverse causes
- Requires specialised intervention
Moments of Insomnia
Initial Insomnia:
- Difficulty falling asleep (takes >30 minutes)
- Often associated with anxiety and worry
- The mind "can't switch off"
Intermediate Insomnia:
- Very light sleep
- Frequent awakenings during the night
- Difficulty falling back asleep
- Related to stress, pain or other medical disorders
Terminal Insomnia:
- Early awakening (typically between 3am-5am)
- Inability to go back to sleep
- Often associated with depression

Causes and risk factors
Neurobiological factors
Sleep is regulated by complex neurobiological systems.
Neurotransmitters - changes and anomalies:
- SerotoninNeurotransmitter crucial for inducing sleep. Low levels are associated with insomnia
- MelatoninHormone that regulates the sleep-wake cycle (wakefulness = being awake). Its production can be altered
- GABAMain inhibitory neurotransmitter in the brain. Deficiency results in brain hyperactivation
- CortisolStress hormone. High levels (especially at night) maintain alertness
Genetic predisposition: Studies show that there is a hereditary component to insomnia, with first-degree relatives presenting a 2-3 times higher risk.
Psychological factors
Stress and anxiety (40-50% of cases):
- Excessive worry about everyday problems
- Suffering in anticipation of not being able to fall asleep
- Mental rumination - repetitive thoughts that don't stop
Depression:
- 75% of people with depression have symptoms of insomnia
- It can be both a cause and a consequence of insomnia
Trauma and post-traumatic stress:
- Hypervigilance that prevents the relaxation needed for sleep
- Nightmares and night fears
- Association of bed/darkness with vulnerability
Environmental and lifestyle factors
Inadequate sleep hygiene:
- Irregular going to bed and getting up times
- Using the bed for activities other than sleeping
- Unsuitable environment (noise, light, temperature)
Use of screens and blue light:
- Blocking the production of melatonin (which induces sleep)
- Brain stimulation before bed
- Associating the bedroom with activity rather than rest
Chemical substances and compounds:
- Caffeine: May affect sleep up to 6-8 hours after consumption
- Alcohol: It's a sedative, but it prevents quality sleep
- NicotineStimulant that makes it difficult to fall asleep
- Stimulant medication: Difficult to fall asleep
Medical conditions:
- Chronic pain (fibromyalgia, arthritis)
- Respiratory problems (asthma, sleep apnoea)
- Gastro-oesophageal reflux
- Hyperthyroidism
- ...

Diagnosing Insomnia
Updated diagnostic criteria
The diagnosis of insomnia is based on well-defined clinical criteria, without the need for specific tests in most cases:
Essential criteria (ICSD-3-TR):
- Complaining of insomniaDifficulty initiating or maintaining sleep, or early awakening
- The right opportunity: Environmental conditions and enough time to sleep
- Daytime losses: Significant impact on daily functioning
- Frequency: At least 3 nights a week
- DurationMinimum 3 months for diagnosis of chronic insomnia
Assessment tools
Sleep diary - detailed record for 1-2 weeks including:
- Time to lie down and get up
- Time to fall asleep
- Number and duration of awakenings
- Sensation on waking
- Sleepiness and daytime functioning
Questionnaires validated for the Portuguese population:
- Pittsburgh Sleep Quality Index (PSQI)
- Epworth Sleepiness Scale
- Basic Insomnia and Sleep Quality Questionnaire (BaSIQS)
PolysomnographyGenerally not necessary for diagnosing insomnia, except when it is suspected:
- Sleep apnoea
- Periodic leg movements
- Other sleep disorders
Important Note:The diagnosis must be always done by a specialised professional. Self-diagnosis can lead to incorrect conclusions and inadequate treatment.

Insomnia's impact on daily life
Insomnia has devastating consequences that extend far beyond simple fatigue, affecting all dimensions of life:
Physical impact
- Compromised immune system: Increased susceptibility to infections
- Increased cardiovascular risk: Hypertension, myocardial infarction
- Type 2 diabetesDifficulty regulating blood sugar levels
- Food compulsions: Imbalance in hunger hormones (leptin and ghrelin)
- Accelerated ageing: Lower production of growth hormone
Cognitive impact
- MemoryDifficulty consolidating new information
- Concentration: Inability to focus on tasks
- Decision-making: Very impaired judgement and increased impulsivity
- Creativity: Reduced problem-solving capacity
Emotional impact
- IrritabilityLow frustration tolerance
- Anxiety: Excessive worry and constant tension
- Depression: 3-4 times greater risk of developing depressive episodes
- Emotional control: Difficulty regulating emotions
Social and professional impact
- Absenteeism from work2-3 times more absences from work
- Accidents: Double risk of road accidents
- Relationships: Marital and family tensions
- Productivity: 20-30% reduction in professional income
Economic impact
- Direct costsmedical appointments, medicines
- Indirect costsloss of productivity, early retirement
- Estimated loss: 1-2% of GDP in developed countries
The Real Impact of Sleep Deprivation - examples
Risk of Alzheimer's
Lack of sleep throughout life is one of the biggest risk factors for Alzheimer's. During deep sleep, the brain cleanses toxins, including beta-amyloid associated with the disease. Margaret Thatcher and Ronald Reagan, known for sleeping only 4-5 hours a night, both developed Alzheimer's.
Cancer
The WHO has classified night work as a probable carcinogen. Lack of sleep is linked to cancers such as bowel, prostate and breast. Just one night of 4 hours of sleep reduces cells by 70% "natural killer" - responsible for eliminating errors in cell division processes - which are crucial in the fight against cancer.
Cardiovascular Diseases
Alarming data on daylight saving time: in spring, when we "lose" 1 hour of sleep, there is a 24% increase in heart attacks the following day. In autumn, when we "gain" 1 hour, there is a decrease of 21%.
Impact on DNA
A week of sleeping 6 hours a night distorts the activity of 711 genes - some of them promote tumours and inflammation, others are responsible for immunity.
General Mortality
The less you sleep, the shorter your life expectancy. Short sleep predicts all-cause mortality.

How is Insomnia treated?
Treating insomnia evolved significantlywith evidence-based approaches that address the underlying causes instead of just masking the symptoms. The multimodal approach is the most effective.
Cognitive Behavioural Therapy for Insomnia (CBT)
A TCCI is considered the first-line treatment for chronic insomnia by all international medical guidelines.
What is TCCI?
- Brief psychotherapeutic intervention (6-8 sessions)
- Addresses thoughts, behaviours and beliefs that perpetuate insomnia
- Based on solid scientific evidence
- Superior efficacy to long-term medication
TCCI components
1. Learning about sleep:
- Understanding normal sleep mechanisms
- Debunking wrong beliefs about sleep
- Setting realistic expectations
2. Sleep hygiene:
- Optimising the environment and behaviour
- Elimination of factors that interfere with sleep
3. Stimulus control:
- Bed only for sleeping and sexual activity
- Get out of bed if you don't fall asleep in 15-20 minutes
- Associate the bedroom with sleep, not wakefulness
4. Sleep restriction:
- Initial limitation of time in bed
- Gradual increase as sleep efficiency improves
- Sleep consolidation
5. Cognitive restructuring:
- Identifying dysfunctional thoughts about sleep
- Replacement with more adaptive thoughts
- Reduction of anticipatory anxiety
Effectiveness of TCCI
- 70-80% of patients experience significant improvement
- 50% reduction in time to fall asleep
- Improvement maintained 12-24 months after treatment
- Superior to medication in long-term efficacy
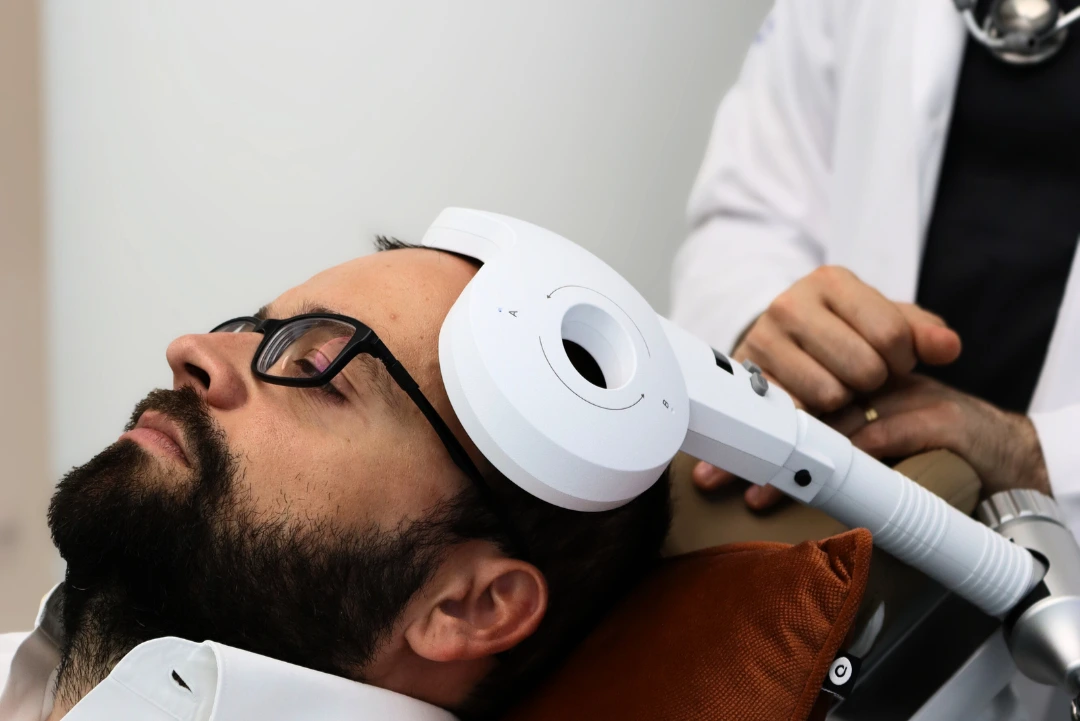
Neurotherapy
A Neurotherapy represents a revolution in the treatment of insomniaoffering effective alternatives without the side effects of medication.
Transcranial Magnetic Stimulation (TMS):
- Modulates the activity of brain areas involved in sleep regulation
- Acts on the prefrontal cortex and limbic system (hormonal)
- 20-30 minute sessions, non-invasive and painless treatment
- Proven effectiveness in academic and clinical studies
Neurofeedback:
- Trains the brain to self-regulate for healthy sleep patterns
- Real-time feedback on brain activity
- Improving the natural ability to relax
- Particularly effective for anxiety-related insomnia
Transcranial Direct Current Stimulation (tDCS):
- Modulates neuronal excitability
- Enhances neuroplasticity
- Effectively complements other treatments
- Benefits continue 2-4 months after treatment
Advantages of Neurotherapy
- No significant side effects
- Not as addictive as medication
- Acts on the neurobiological causes of insomnia
- Lasting improvement even after the end of treatment
- Combinable with other therapeutic approaches
Pharmacological treatment
Although should not be the first-line treatmentmedication can be useful in specific situations:
When to consider?
- Acute insomnia during crises
- Failure of non-pharmacological treatments
- Severe insomnia with serious functional impact
- As a bridge to other treatments
Types of medicines
- Short-acting hypnotics:
- Zolpidem, zopiclone
- Quick start, quick disposal
- Less risk of daytime sleepiness
- Sedative antidepressants:
- Trazodone, mirtazapine
- Useful when there is a parallel diagnosis of depression/anxiety
- Profile of side effects to consider
- Antihistamines:
- Diphenhydramine, doxylamine
- Available without prescription
- Limited efficacy, builds tolerance quickly
- Benzodiazepines:
- Short-term effectiveness
- High risk of dependence and tolerance
- Negative effects on sleep architecture
- Contraindicated for prolonged use
Medication problems
- Dependence and tolerance: Need for progressively higher doses
- Bounce effect: Insomnia worsens when medication is stopped
- Daytime sleepiness: Impact on operation
- Altered sleep architecture: Less restful sleep
- Medicinal mixtures: Especially in the elderly
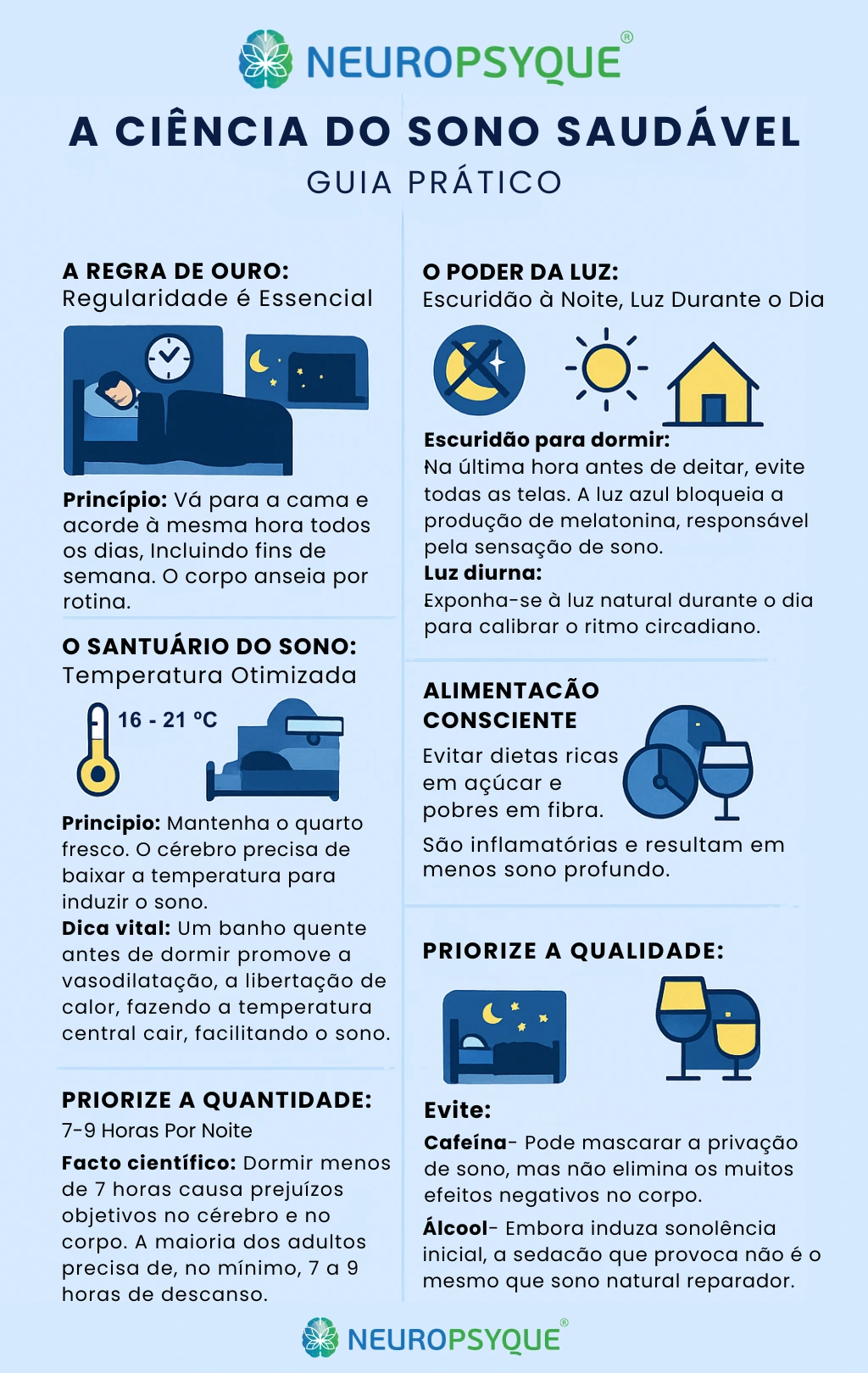
The Science of Healthy Sleep - A Practical Guide
1. The Golden Rule: Regularity is Essential
Principle: Go to bed and wake up at the same time every day, including weekends. Your body craves routine.
Why: Regularity reinforces the circadian rhythm, optimising the production of hormones and biological processes.
2. The Power of Light: Dark at Night, Light by Day
Darkness to sleep:
- In the last hour before bed, avoid all screens
- Blue light suppresses melatonin for around 3 hours and reduces its peak at 50%
Daylight:
- Expose yourself to natural light during the day to calibrate your circadian rhythm
3. The Sleep Sanctuary: Optimised Temperature
Principle: Keep the room cool. The brain needs to lower its temperature by 1-1.5°C to initiate sleep.
Top tip: A hot bath before bed works by vasodilating - when you get out, you release a lot of heat, causing your core temperature to drop and making it easier to fall asleep.
4. Conscious eating
Avoid: Diets high in sugar and low in fibre impair sleep, resulting in less deep sleep.
Timing: Last meal about 2 hours before bedtime.
5. Prioritise Quantity: 7-9 Hours Per Night
Scientific fact: Sleeping less than 7 hours causes objective damage to the brain and body. Most adults need 7-9 hours.
6. Beware of stimulants
Caffeine: It can mask sleep deprivation but it doesn't eliminate the underlying negative effects on the body.
Alcohol: Although it induces initial drowsiness, sedation is not the same as natural restful sleep.

When to seek professional help
It is essential to seek specialised assessment when symptoms begin to significantly interfere with daily functioning.
Don't wait for the condition to worsen.
Signs to seek help
- Sleep difficulties 3 or more nights a week for more than 1 month
- Time to fall asleep consistently longer than 30 minutes
- Frequent awakenings (more than twice a night) with difficulty getting back to sleep
- Wake up at least 2 hours earlier than desired
- Feeling of unrefreshing sleep even when sleeping 7-8 hours
- Fatigue during the day that interferes with ordinary activities
- Irritability, anxiety or depression
- Concentration or memory difficulties
- Constant worry about sleep
- Regular use of sleep medication or alcohol
When it's urgent
- Suicidal thoughts related to exhaustion
- Accidents due to drowsiness
- Total inability to work
- Psychotic symptoms related to sleep deprivation
- Abuse of sleeping substances

Advances in scientific research
Insomnia research is evolving rapidly, bringing new hope to those who suffer from the condition.
Discoveries about the brain
Recent studies show that people with insomnia have an "always-on" brain. The brain can't switch off completely, even during sleep. Scientists have also discovered specific genes that control sleep, which could lead to personalised treatments in the future.
New forms of treatment
Digital therapies
In 2024, the FDA approved the first digital device for insomnia - Sleepio Rx. It's an app that teaches you techniques to sleep better. Studies show that 76% of the people who used it were able to sleep better.
Brain stimulation
New devices that gently stimulate the brain are showing promising results:
- Portable TMS: Uses magnetic fields to help the brain relax
- Electrical stimulation: Devices worn on the forehead that help you fall asleep faster
- Modius Sleep: A device approved in 2024 that is worn as headphones and improves sleep in 95% of people
New medicines
Safer drugs are emerging that act differently from traditional ones. These new drugs block the substances in the brain that keep us awake, rather than forcing sleep.
The future
In the coming years, insomnia treatment will become more personalised. Devices such as smart watches will help predict sleep problems before they happen.

Myths and Truths about Insomnia
| Myth | Truth |
| "Insomnia is a lack of discipline" | It's a real medical condition with a proven neurobiological basis. |
| "8 hours are compulsory" | Needs vary between 6-10 hours. Quality is more important than absolute quantity. |
| "Alcohol helps you sleep" | It induces drowsiness but fragments sleep and significantly reduces its quality. |
| "Medication always solves the problem" | Medication can help, but it hardly solves the problem. CBT, neurotherapy and information technology get to the root of the problem. |
Resources and support available in Portugal
Portugal has several resources and organisations dedicated to supporting people with insomnia.
| Resource | Description |
| Portuguese Sleep Association | National organisation dedicated to ADHD, offering information and support |
| National Health Service (SNS) | Child psychiatry, psychiatry and neurology consultations through the family doctor |
| SNS 24 line | 24-hour telephone support: 808 24 24 24 |
| University Hospitals | Specialised consultations on ADHD and neurodevelopmental disorders |
| Local Associations | Regional and local support groups |
In NeuroPsyqueWe are part of a network of specialised care, offering a response that combines Neurology, Neuropsychology e Neurotherapy.
Our commitment is, as always, to provide you with the greatest possible expectation of improvement.
We have the most specialised equipment and specialists in therapies such as NeuroFeedback, a Transcranial Magnetic Stimulation and Transcranial Electrical Stimulation, which have proved important in the treatment of insomnia. Book your appointment with us!
Conclusion
With advances in CBT and neurotherapy, we now have effective tools that address the root of the problem, bringing about lasting improvements.
Vital message: Sleep is not optional - it is a fundamental biological need. Chronic sleep deprivation not only reduces quality of life, but dramatically increases the risk of serious illness and early death.
Book an appointment with us and find out how we can help you sleep better and live better!
Questions and answers about Insomnia
1. Can insomnia be cured?
Insomnia is highly treatable. With TCCI and neurotherapy, 70-80% of patients experience significant improvement. The aim is to restore normal sleep patterns.
2. How long does the treatment take?
TCCI: 6-8 sessions over 2-3 months. Neurotherapy: Benefits after 5-10 sessions, full treatment 15-20 sessions.
3. Can I treat insomnia without medication?
Yes. As well as being possible, it is recommended and less risky. CBT is more effective than medication in the long term, and neurotherapy offers lasting results without side effects.
4. Is neurotherapy effective for insomnia?
Yes, multiple studies have shown the effectiveness of EMT e Neurofeedback. They act directly on the brain circuits responsible for sleep regulation.
5. How many hours of sleep do I really need?
Most adults need 7-9 hours. Sleeping less than 7 hours already causes objective damage to the brain and body.
6. Does alcohol really help you sleep?
No. Although it induces initial drowsiness, alcohol significantly fragments sleep and blocks restorative REM sleep.
7. How do I know if I need professional help?
If you've had difficulties 3+ nights a week for more than a month, or if your sleep affects your daily functioning. Early diagnosis improves prognosis.
8. Does screen light really affect sleep?
Yes, drastically. Blue light suppresses melatonin for around 3 hours and reduces its peak at 50%. Avoid screens in the last hour before bed.
9. Is room temperature important?
Fundamental. The brain needs to drop 1 to 2 °C (degrees) to start sleeping. Cool rooms facilitate this natural process.
10. Are naps harmful?
Short naps (20-30 min) before 3pm can be beneficial. They should not consistently compensate for insufficient night-time sleep.
11. Does caffeine affect sleep?
Yes, significantly. Caffeine can mask deprivation but it doesn't eliminate the underlying negative effects. Avoid after midday.
12. What is the relationship between insomnia and serious illnesses?
Direct and alarming. Insomnia increases the risk of Alzheimer's, cancer, cardiovascular disease and reduces life expectancy. A 4-hour night's sleep reduces anti-cancer cells by 70%.





